February 06, 2007
Dermatomyositis

Posted by mmw at 06:56 PM | Comments (0)
September 25, 2006
Antinuclear antibody patterns
OVERVIEW
• Antinuclear antibodies (ANA): autoantibodies directed against histones, double-stranded and single-stranded DNA, ribonucleoprotein (RNP) complexes, and other nuclear components.
• Indirect immunofluorescence assays detect antibodies that bind to various nuclear antigens, and are used to report the titer of the ANA and the pattern of nuclear staining of the ANA.
• Titers 1:40 are considered positive.
• Titers 1:320 are more likely to represent true-positive results.
• There are various staining patterns
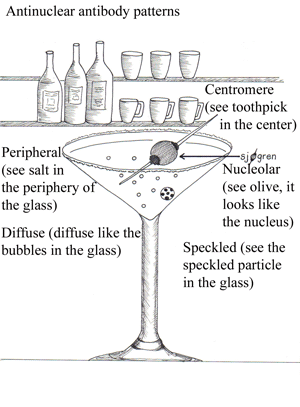
STAINING PATTERNS
• Diffuse / homogeneous: antibodies to histone (see bubbles in glass “think of histone subunits floating in the glass”)
• Rim: antibodies to nuclear envelope proteins and to double-stranded (ds) DNA (see salt on the rim of the glass)
• Speckled: antibodies to Sm, RNP, Ro/SS-A, La/SS-B, and other antigens (see speckled particle in the glass)
• Nucleolar: associated with diffuse scleroderma
• Centromeric: highly specific for the CREST syndrome
ANTIBODIES TO HISTONE
• Drug induced lupus: Anti-histone antibodies are sensitive but nonspecific for drug-induced lupus
• Anti-histone antibody testing may be useful in patients with a positive ANA test and a history of exposure to medications associated with drug-induced lupus (i.e. procainamide, isoniazid, hydralazine).
ANTIBODIES TO DOUBLE-STRANDED DNA (dsDNA)
• Antibodies to dsDNA recognize its base pairs, its ribose-phosphate backbone, and the structure of its double helix
• Systemic Lupus Erythematous (SLE): High titers of anti-double-stranded DNA (anti-dsDNA) antibodies are highly specific SLE (present in 60% of patients with SLE)
• Antibodies to dsDNA should be measured when there is clinical suspicion of SLE and the ANA is positive
• Specificity of anti-dsDNA antibodies for SLE is 97% overall and approaches 100% when the antibody titer is high
ANTI-SMALL NUCLEAR RIBONUCLEOPROTEINS
• Anti-Sm (anti-Smith) antibodies: specific for SLE (20 - 30 % of SLE patients)
• Anti-U1 snRNP : SLE (30 - 40 %); myositis; esophageal hypomotility; sclerodactyly; Raynaud's phenomenon; arthralgias; arthritis; and mixed connective tissue disease (MCTD)
• Testing for anti-U1 snRNP should be limited to patients with a positive ANA test who are suspected of having SLE or MCTD
ANTI- Ro/SS-A and ANTI -La/SS-B
• Antibodies to La almost always occur in association with anti-Ro antibodies
• Anti-Ro/SS: Primary Sjögren's syndrome (SS); positive in 40-50%
• Anti-La : SLE (10 to 15 percent of patients); late-onset SLE; secondary Sjögren's syndrome; congenital complete heart block (90%);and neonatal lupus syndrome (70%)
• RNA-protein conjugates
• Ro and La refer to the antigen as localized to the cytoplasm
• SS-A and SS-B are nuclear antigens
ANTI-CENTROMERE
• Antibody to the kinetechore of chromosomes
• Scleroderma (22 – 36%)
• Raynaud's phenomenon
• CREST syndrome (15%)
• Primary biliary cirrhosis
Posted by mmw at 05:58 PM | Comments (0)
May 30, 2006
Still's disease
DISEASE OVERVIEW
• Still's disease is a form of arthritis that is characterized by high spiking fevers and transient
salmon-colored rash.
• First described in children, but it is now known to occur, much less commonly, in adults
• Possible Pathogenesis: Infection; hypersensitivity; or autoimmune disorder
SIGNS and SYMPTOMS
• Extreme fatigue
• Waves of high fever 104 degrees F (41 degrees C)
• Faint salmon color skin rash comes and goes usually doesn’t itch.
• Inflammation of the lungs (pleuritis)
• Inflammation of the pericardium (pericarditis)
• Fluid accumulation around the lung (pleural effusion)
• Inflammation of the liver
• Sore throat
• Arthritis this usually involves many joints (polyarticular arthritis).
DIAGNOSIS
• Persistent arthritis (arthritis lasting at least 6 weeks)
• Markedly elevated white blood cell count
• Low red blood count (anemia)
• Elevated ESR
• Rheumatoid arthritis (rheumatoid factor) and systemic lupus erythematosus (antinuclear antibodies, ANA) are usually negative. Other diseases especially infections, cancer, and other types of arthritis are excluded

TREATMENT
• Aspirin or other non-steroid drugs (NSAIDs)
• Steroids such as prednisone, are used to treat more severe features of illness.
• Persistent illness: medications that affect the inflammatory aspects of the immune system are used.
These include:
• Hydroxychloroquine (Plaquenil)
• Penicillamine
• Azathioprine (Imuran)
• Methotrexate (Rheumatrex)
• Cyclophosphamide
• Etanercept (Enbrel)
• Infliximad (Remicade)
• Corticosteroids
Posted by mmw at 01:16 PM | Comments (0)
February 09, 2006
Osteoarthritis
DISEASE OVERVIEW
• Osteoarthritis (OA ) is degenerative disease more common in older adults
• Approximately one millon people affected
• Morning stiffness less than 30 minutes
• Pain exacerbated with movement
• Rare systemic involvement
DIAGNOSIS
• Minimal joint inflammation
• Bony enlargement of the affected joint
• Pain and/or deformity in the distal and proximal interphalangeal joints (DIP and PIP)
(see figures 1A and 1B)
• Radiographic findings: narrowing joint space; osteophyte formation; sharpened articular margins; dense subchondral bone (absence of radiographic findings does not exclude the diagnosis)
SIGNS
• Nodes: bony enlargements of the affected joints
• BOUCHARD nodes occur at the PIP joint (think of a BUTCHER grasping the knife using his PIP joint
as he chops meat; see Fig. 1A)
• HEBERDEN nodes occur at the DIP joint (think of a gardener picking HERBS using his DIP joints)
• Limited range of motion
• Crepitus on motion

Heberden nodes occur at the DIP joint (Think of a gardener flexing his DIP joints while picking herbs)

TREATMENT
• Nonpharmacological: weight reduction; exercise; and joint protection.
• Initial pharmacological treatment: acetaminophen and capsaicin, (.025%)
• Moderate pain: Non steroidal anti-inflammatory agents (NSAIDS).
• Severe pain: steroid injections( ie. 40mg Triamcinolone) into the most severely affected joint;
Hyaluronic acid-like product joint injections
• Surgical intervention: joint replacements for moderate to severe pain and functional impairment
.
Posted by mmw at 08:54 PM | Comments (0)