February 06, 2007
Dermatomyositis

Posted by mmw at 06:56 PM | Comments (0)
September 25, 2006
Antinuclear antibody patterns
OVERVIEW
• Antinuclear antibodies (ANA): autoantibodies directed against histones, double-stranded and single-stranded DNA, ribonucleoprotein (RNP) complexes, and other nuclear components.
• Indirect immunofluorescence assays detect antibodies that bind to various nuclear antigens, and are used to report the titer of the ANA and the pattern of nuclear staining of the ANA.
• Titers 1:40 are considered positive.
• Titers 1:320 are more likely to represent true-positive results.
• There are various staining patterns
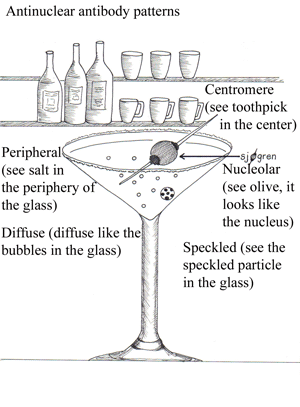
STAINING PATTERNS
• Diffuse / homogeneous: antibodies to histone (see bubbles in glass “think of histone subunits floating in the glass”)
• Rim: antibodies to nuclear envelope proteins and to double-stranded (ds) DNA (see salt on the rim of the glass)
• Speckled: antibodies to Sm, RNP, Ro/SS-A, La/SS-B, and other antigens (see speckled particle in the glass)
• Nucleolar: associated with diffuse scleroderma
• Centromeric: highly specific for the CREST syndrome
ANTIBODIES TO HISTONE
• Drug induced lupus: Anti-histone antibodies are sensitive but nonspecific for drug-induced lupus
• Anti-histone antibody testing may be useful in patients with a positive ANA test and a history of exposure to medications associated with drug-induced lupus (i.e. procainamide, isoniazid, hydralazine).
ANTIBODIES TO DOUBLE-STRANDED DNA (dsDNA)
• Antibodies to dsDNA recognize its base pairs, its ribose-phosphate backbone, and the structure of its double helix
• Systemic Lupus Erythematous (SLE): High titers of anti-double-stranded DNA (anti-dsDNA) antibodies are highly specific SLE (present in 60% of patients with SLE)
• Antibodies to dsDNA should be measured when there is clinical suspicion of SLE and the ANA is positive
• Specificity of anti-dsDNA antibodies for SLE is 97% overall and approaches 100% when the antibody titer is high
ANTI-SMALL NUCLEAR RIBONUCLEOPROTEINS
• Anti-Sm (anti-Smith) antibodies: specific for SLE (20 - 30 % of SLE patients)
• Anti-U1 snRNP : SLE (30 - 40 %); myositis; esophageal hypomotility; sclerodactyly; Raynaud's phenomenon; arthralgias; arthritis; and mixed connective tissue disease (MCTD)
• Testing for anti-U1 snRNP should be limited to patients with a positive ANA test who are suspected of having SLE or MCTD
ANTI- Ro/SS-A and ANTI -La/SS-B
• Antibodies to La almost always occur in association with anti-Ro antibodies
• Anti-Ro/SS: Primary Sjögren's syndrome (SS); positive in 40-50%
• Anti-La : SLE (10 to 15 percent of patients); late-onset SLE; secondary Sjögren's syndrome; congenital complete heart block (90%);and neonatal lupus syndrome (70%)
• RNA-protein conjugates
• Ro and La refer to the antigen as localized to the cytoplasm
• SS-A and SS-B are nuclear antigens
ANTI-CENTROMERE
• Antibody to the kinetechore of chromosomes
• Scleroderma (22 – 36%)
• Raynaud's phenomenon
• CREST syndrome (15%)
• Primary biliary cirrhosis
Posted by mmw at 05:58 PM | Comments (0)
August 11, 2006
Cholesterol lowering drugs
Cholesterol treatment guidlines:
Current guidelines for cholesterol treatment: http://www.nhlbi.nih.gov/guidelines/cholesterol/profmats.htm
Drug Treatment:
There are four major classes of medications are used to treat hyperlipidemia:
o HMG-CoA reductase inhibitors (statins)
o Bile acid sequestrants (cholestyramine, cholestipol)
o Nicotinic acid
o Fibric acids

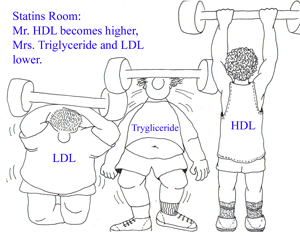
o The statins can lower LDL levels by 18% to 55% and triglyceride levels by 7% to 30%. They also can raise HDL levels by 5% to 15%.Their major side effects include myopathy and an elevation of liver enzyme levels.
o The bile acid resins (cholestyramine, cholestipol) lower LDL levels by 15% to 30%, and raise HDL levels by 3% to 5%. They have no effect on triglyceride levels. Their major side effects include gastrointestinal distress, constipation, and a decrease in the absorption of other drugs.
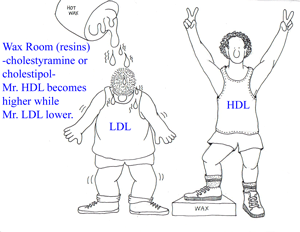
o Nicotinic acid lowers LDL levels by 5% to 25% and triglyceride levels by 20% to 50%. Nicotinic acid also raises HDL levels by 15% to 35%. The major side effects of nicotinic acid include flushing, hyperglycemia, hyperuricemia, GI distress, and hepatotoxicity.
o Fibric acids lower LDL levels by 5% to 20% and triglyceride levels by 20% to 50%, and raise HDL levels by 10% to 20%. Their major side effects include dyspepsia, gallstones, myopathy, and unexplained noncardiac death.
Posted by mmw at 09:39 PM | Comments (0)
October 05, 2005
VonRecklingenhausen Disease
HISTORICAL INFORMATION
• 1793: Tilesius von Tilenau first described neurofibromatosis.
• 1849: R. W. Smith further described it.
• 1882: von Recklinghausen was the first person to associate the origin of this disorder to tumors
arising from cells of the nerve sheaths.
• 1880s: Joseph Carey Merrick in London known as the “elephant man” because of his disfiguring
deformity of the head, extremities, and vertebral column.
DISEASE OVERVIEW
• Type 1 neurofibromatosis (NF1, von Recklinghausen disease, peripheral neurofibromatosis) is a
multisystemic disease.
• autosomal dominant disorder; Chromosome 17 gene locus
(17 letters in VonRecklingenhausen disease)
• 1 in 4000 individuals are affected.
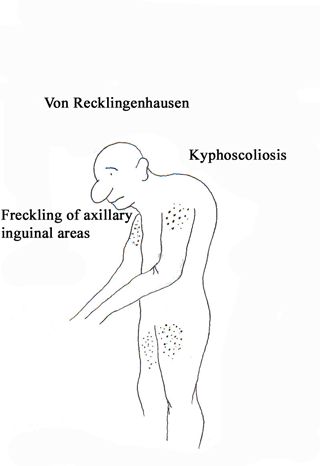
DIAGNOSIS (2 or more of the following criteria)
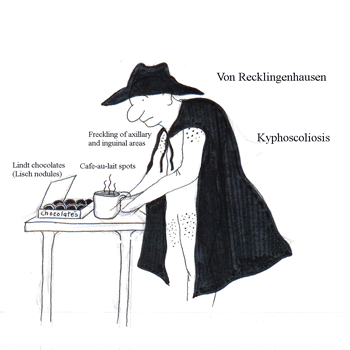
• More than 6 café-au-lait spots measuring at least 15 mm in adults and 5 mm in children
(Café-au-lait spots are found in more than 50% of individuals with NF1.)
• At least 2 or more neurofibroma of any type or at least 1 plexiform neurofibroma
• Freckling in the axillary or inguinal regions
• Optic glioma
• Two or more Lisch nodules (iris hamartomas) (VonRecklingenhausen is eating Lindt chocolates)
• A distinctive bony lesion, such as sphenoid wing dysplasia or thinning of a long bone with or
without pseudoarthrosis
• A first-degree relative with NF1, as suggested by these criteria
SIGNS
• spinal deformities: scoliosis and kyphoscoliosis.
• congenital bowing and pseudoarthrosis of the tibia and the forearm.
• overgrowth phenomenon of the extremity.
• soft tissue tumors
TREATMENT
• Plastic surgery to correct disfigurement
• Surgical treatment of intraspinal or intracranial tumors, and tumors of the peripheral nerve
Posted by mmw at 06:21 PM | Comments (0)